Laparoscopic Robotic Surgery Kansas City
A prolapse occurs when surrounding organs or structures push into your vaginal canal, often causing urinary problems, bowel symptoms, and sexual dysfunction, among other issues. If you’re struggling with a prolapse, Patrick Nosti, MD, FACOG, at Urogynecology of Kansas City, offers innovative treatment solutions. Find out more by booking a prolapse evaluation today.
UROGYNECOLOGY OF KANSAS CITY | 913.262.3000
 High-Volume DaVinci Robotic Surgeon
High-Volume DaVinci Robotic Surgeon
Gynecologic robotic surgery is one of the latest innovations in minimally invasive surgical techniques. Using a narrow, lighted scope and miniature instruments controlled through a robotic system, Dr. Nosti is able to treat several conditions.
With traditional open surgery, surgeons make one long incision to access the area for treatment. With laparoscopic surgery, surgeons hold and manipulate a scope and instruments through a few small incisions. Robotic surgery is similar to laparoscopy, with the main difference being in how surgeons control the surgical tools.
Dr. Nosti has the highly specialized training necessary to perform these advanced robotic procedures. Because he has performed hundreds of them, he is able to ensure patients have the best possible results.
Robotic-assisted sacrocolpopexy
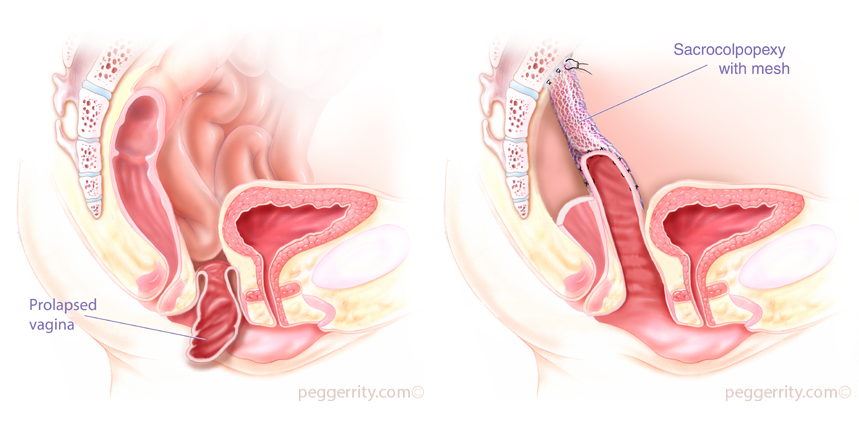
Sacrocolpopexy is one of the most successful operations used to correct vaginal vault prolapse, and it is considered by many to be the “gold standard”. It involves attaching one end of a synthetic mesh to the top of the vagina and the other end to the sacral promontory (upper part of the tailbone or lower part of the spine), thereby restoring the vagina to its normal anatomic position.
Robotic sacrocolpopexy represents a state-of-the-art, minimally invasive approach to the surgical correction of vaginal vault prolapse. And for most women, this translates into many benefits, including:
- Shorter hospital stay
- Less pain
- Less blood loss and transfusions
- Less scarring
- Faster recovery
- Quicker return to normal activities
Robotic-Assisted Hysterectomy
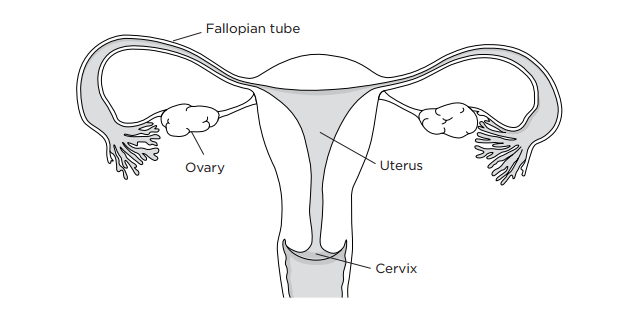
Your uterus is located in the lower abdomen (belly) between your bladder and rectum. The lower, narrow end of your uterus is called your cervix. Your ovaries and fallopian tubes are attached to your uterus.
After your hysterectomy, you will not be able to have children naturally. Menstruation (getting your period) will also stop. A hysterectomy does not cause menopause unless your ovaries are removed.
During a Robotic-assisted hysterectomy, the surgeon will make several small incisions (surgical cuts) on your abdomen. A laparoscope (a tube-like instrument with a camera) will be placed into your abdomen. The tool is connected to a video camera and television that allow your surgeon to see the inside of your abdomen. Gas (carbon dioxide) will be pumped into your abdomen to create space, which gives your surgeon more room to perform the surgery. Tiny tools will also be inserted into the incisions in your abdomen. The surgeon uses a robot as a tool to do the surgery. Your surgeon sits at a console with a 3-dimensional view of the surgical site. They do the surgery from there, using a robot that they control.
The surgeon removes your uterus and cervix through your vagina, if possible. If your uterus or cervix can’t be removed through your vagina, your surgeon will make one of your incisions larger and remove the organs from there. Your incisions will be closed with sutures (stitches). In some cases, the cervix is left in place. Your surgeon will discuss the implications of this approach, including its risks and benefits.

Salpingo-Oophorectomy
Depending on your surgery, one or both of your ovaries and fallopian tubes may be removed. This is called a salpingo-oophorectomy. If both ovaries are removed, you will go into menopause if you have not already. If you have already gone through menopause, you should not notice any changes. If you have not started menopause, you may experience common symptoms, including night sweats, hot flashes, and vaginal dryness. Speak with your doctor about ways to manage these symptoms.
Related Reviews
Very Professional | 5.0 
“The staff is all very friendly and helpful. Dr Nosti explains options in simple terms that are easily understood. Surgical experience before & after was great!“
Review from David Faircloth | Source: Google | September 10th, 2020
How Much Does Laparoscopic & Robotic Surgery Cost?
The cost of Laparoscopic and Robotic Surgery in Kansas City will depend on several factors. The price can be affected by body type, type of technique performed, surgical complications, and even allergies. Find out more by scheduling a consultation.
Schedule a Consultation
Schedule your consultation for Laparoscopic Robotic Surgery in Kansas – contact Dr. Nosti and set up your appointment. During your appointment, you will be able to ask questions and bring up any concerns you may have about the procedure. Contact us today to get the look you’ve always wanted!
